Table of Contents
Analysis of the Factors of Therapeutic Failure after Transition to Acriptega: About Two Cases
Published on: 20th February, 2026
Acriptega, a combination of Dolutegravir, Lamivudine, and Tenofovir, is a cornerstone of modern antiretroviral therapy due to its efficacy and tolerability. However, treatment failures persist despite this optimization, raising questions about barriers to successful treatment. Through the analysis of two clinical cases, this study explores the biological and behavioral factors contributing to these failures following a switch to this molecule.The first case is a 69-year-old female patient, diagnosed with HIV in 2002 following pulmonary tuberculosis, who was regularly monitored with an undetectable viral load and a CD4 count > 500 cells/mm³ until the Acriptega transition and the onset of tumor symptoms in 2024. The second case is a 62-year-old female patient, diagnosed with HIV in 2009 following cerebral toxoplasmosis. She was regularly monitored with good treatment adherence and an undetectable viral load. After switching her triple therapy, she developed gastroenteritis, which led to the discovery of her treatment failure. This case study highlights that failure after switching to Acriptega is linked to the absence of prior resistance testing (genotyping). A safe switchover requires a rigorous assessment of the patient’s virological history to prevent the emergence of cross-resistance. Close monitoring via genotyping is essential.
Bacteriolysis Destruction for Cu- and Zn-Ions Induced Peptidoglycan Cell Wall Based on the Halo-test Results in Cu(NO3)2 and ZnSO4 Solutions against Staphylococcus epidermidis
Published on: 24th March, 2026
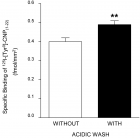
Bacteriolysis of peptidoglycan (PGN) cell wall destruction on cleavage, hydrolysis, and decomposition by copper nitrate and zinc sulfide solutions has been investigated on the ground of the results obtained from halo antibacterial susceptibility tests in metal sulfate solutions against Staphylococcus epidermidis, in which from halo-antibacterial susceptibility tests of metallic ion concentration of 100 mM/L against Staphylococcus epidermidis, the order of bacterial effect for the metal nitrate solutions is as follows, Cu2+>Zn2+ >Ag+>Pb2+>Al3+, and the other, in the metal sulfate solutions, the antibacterial effect order is found to be Zn2+>Cu2+>Ag+>Al3+. Cu(Ⅱ)-, Zn(Ⅱ)-ions induced bacteriolytic destructions for PGN cell wall on cleavage, hydrolysis, and decomposition within Cu(NO3)2 and ZnSO4 solutions have been elucidated that Cu(Ⅱ) and Zn(Ⅱ) ions can inhibit PGN biosynthesis Transpeptidase (TP)/Trans-glycosylase (TG) and PGN elongation, PGN cleavage occurs by copper ions- and zinc ions-containing autolysins amidase; AmiE, Rv3717, AmiA, PGN cell wall is hydrolyzed by copper-, and zinc-containing enzymes; PGRPs, MurA, LytA, LytM=Endopeptidase, Hydrolase LytB, and PGN decomposition by copper-, zinc-containing PGN inhibitive elongation occurs. Thus, Cu(Ⅱ) and Zn(Ⅱ) within Cu(NO3)2 and ZnSO4 solutions inhibit PGN biosynthesis and activate bacterial PGN autolysins against Staphylococcus epidermidis.
Global Burden and Future Outlook of Antimicrobial Resistance
Published on: 25th March, 2026
Antimicrobial resistance (AMR) is a serious global health crisis. It is getting worse every year. Low- and middle-income countries (LMICs) are the most affected. This is mainly because infectious diseases are very common there. Poor water, sanitation, and hygiene (WASH) systems make things worse. On top of that, vaccination rates in these countries remain very low. All these factors together make AMR a much bigger threat in LMICs than anywhere else.The recent data showed that bacterial AMR was linked to about 4.95 million deaths worldwide, and 1.27 million of the deaths were directly attributable in 2019. Using information from the Global Burden of Diseases, Injuries and Risk Factors Study 2021. The GBD Antimicrobial Resistance Collaborators employed statistical modelling to evaluate AMR trends from 1990 to 2021 and to forecast the burden through 2050 across 204 nations and territories.The results are concerning. AMR-related deaths have increased significantly. Older adults aged 70 and above are the most affected group. However, there is some good news too. Deaths among children under five have dropped by nearly 50%. This is a big achievement. Better infection prevention has played a major role in this. Vaccination programs have also made a real difference. Improved water and sanitation (WASH) initiatives have helped as well. These combined efforts have clearly saved many young lives.Key pathogens contributing to AMR mortality include Klebsiella pneumoniae, Escherichia coli, Streptococcus pneumoniae and meticillin-resistant Staphylococcus aureus (MRSA). In the absence of improved interventions, deaths attributable to AMR are anticipated to rise to 1.91 million annually by 2050. It is important to strengthen infection prevention, surveillance, vaccination, and WASH with integrated One Health approaches to ease the future impact of AMR.
The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain Syndrome
Published on: 13th April, 2026
The prevailing dogma regarding urinary tract sterility has been fundamentally challenged by advances in culture-independent molecular techniques. The urinary microbiome, also known as the urobiome, is defined as a complex ecosystem comprising bacteria, fungi, and viruses. This microbiome plays a pivotal role in maintaining urological health. Emerging evidence suggests a potential link between urinary microbial dysbiosis and the pathogenesis of Urologic Chronic Pelvic Pain Syndrome (UCPPS), a clinical umbrella term that explicitly encompasses two major phenotypes: Interstitial Cystitis/Bladder Pain Syndrome (IC/BPS) and Chronic Prostatitis/Chronic Pelvic Pain Syndrome (CP/CPPS).This review examines the paradigm shift in understanding urinary tract microbiology, characterizes the urobiome in health and disease, and explores the therapeutic implications of microbiome-targeted interventions for UCPPS management.

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."