Abstract
Case Report
The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain Syndrome
Mohammed Amine Elafari*, Mohammed Amine Bibat, Mamad Ayoub, Amine Slaoui, Tarik Karmouni, Abdelatif Koutani and Khalid Elkhader
Published: 13 April, 2026 | Volume 9 - Issue 1 | Pages: 022-026
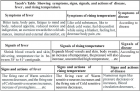
The prevailing dogma regarding urinary tract sterility has been fundamentally challenged by advances in culture-independent molecular techniques. The urinary microbiome, also known as the urobiome, is defined as a complex ecosystem comprising bacteria, fungi, and viruses. This microbiome plays a pivotal role in maintaining urological health. Emerging evidence suggests a potential link between urinary microbial dysbiosis and the pathogenesis of Urologic Chronic Pelvic Pain Syndrome (UCPPS), a clinical umbrella term that explicitly encompasses two major phenotypes: Interstitial Cystitis/Bladder Pain Syndrome (IC/BPS) and Chronic Prostatitis/Chronic Pelvic Pain Syndrome (CP/CPPS).
This review examines the paradigm shift in understanding urinary tract microbiology, characterizes the urobiome in health and disease, and explores the therapeutic implications of microbiome-targeted interventions for UCPPS management.
Read Full Article HTML DOI: 10.29328/journal.ijcmbt.1001036 Cite this Article Read Full Article PDF
Keywords:
Urinary microbiome; Urobiome; Chronic pelvic pain syndrome; IC/BPS; CP/CPPS; Dysbiosis; Metagenomics; Urological disorders
References
- Wei CR, Basharat Z, Osama M, Mah K, Waheed Y, Hassan SS. An overview of the association of the urinary tract microbiome with various diseases and implications for therapeutics. Mini Rev Med Chem. 2025:MRMC-EPUB-150499. Available from: https://doi.org/10.2174/0113895575398906250825113635
- Robino L, Navarro N, Canales-Huerta N, González MJ, Cruz E, Sauto R, et al. Urogenital microbiome, intracellular bacterial communities, and their contribution to urinary tract infections. Microbiol Spectr. 2025:e0124725. Available from: https://doi.org/10.1128/spectrum.01247-25
- Pastuszka A, Tobor S, Łoniewski I, Wierzbicka-Woś A, Sielatycka K, Styburski D, et al. Rewriting the urinary tract paradigm: the urobiome as a gatekeeper of host defense. Mol Biol Rep. 2025;52(1):497. Available from: https://doi.org/10.1007/s11033-025-10609-w
- Roth RS, Liden M, Huttner A. The urobiome in men and women: a clinical review. Clin Microbiol Infect. 2023;29(10):1242-1248. Available from: https://doi.org/10.1016/j.cmi.2022.08.010
- Brubaker L, Putonti C, Dong Q, Wolfe AJ. The human urobiome. Mamm Genome. 2021;32(4):232-238. Available from: https://doi.org/10.1007/s00335-021-09862-8
- Gasiorek M, Hsieh MH, Forster CS. Utility of DNA next-generation sequencing and expanded quantitative urine culture in diagnosis and management of chronic or persistent lower urinary tract symptoms. J Clin Microbiol. 2019;58(1):e00204-19. Available from: https://doi.org/10.1128/jcm.00204-19
- Neugent ML, Hulyalkar NV, Nguyen VH, Zimmern PE, De Nisco NJ. Advances in understanding the human urinary microbiome and its potential role in urinary tract infection. mBio. 2020;11(2):e00218-20. Available from: https://doi.org/10.1128/mbio.00218-20
- Moustafa A, Li W, Singh H, Moncera KJ, Torralba MG, Yu Y, et al. Microbial metagenome of urinary tract infection. Sci Rep. 2018;8(1):4333. Available from: https://doi.org/10.1038/s41598-018-22660-8
- Zhang Y, Wang H, Yan R, Wang K, Man J, Yang L. Research advances on the urinary microbiome in non-infectious urinary tract diseases: from community composition to clinical prospects. Front Cell Infect Microbiol. 2026;16:1728182. Available from: https://doi.org/10.3389/fcimb.2026.1728182
- Hashemi N, Tondro Anamag F, Javan Balegh Marand A, Rahnama'i MS, Herizchi Ghadim H, Salehi-Pourmehr H, et al. A systematic and comprehensive review of the role of microbiota in urinary chronic pelvic pain syndrome. Neurourol Urodyn. 2024;43(8):1859-1882. Available from: https://doi.org/10.1002/nau.25550
- Fu C, Zhang Y, Liang L, Lin H, Shan K, Liu F, et al. The microbiota in patients with interstitial cystitis/bladder pain syndrome: a systematic review. BJU Int. 2024;134(6):869-880. Available from: https://doi.org/10.1111/bju.16439
- Shoskes DA, Altemus J, Polackwich AS, Tucky B, Wang H, Eng C. The urinary microbiome differs significantly between patients with chronic prostatitis/chronic pelvic pain syndrome and controls as well as between patients with different clinical phenotypes. Urology. 2016;92:26-32. Available from: https://doi.org/10.1016/j.urology.2016.02.043
- Deng AQ, Yue SY, Niu D, Zhang DD, Hou BB, Zhang L, et al. The role of microbiota in the chronic prostatitis/chronic pelvic pain syndrome: a review. Front Microbiol. 2025;16:1488732. Available from: https://doi.org/10.3389/fmicb.2025.1488732
- Qin J, Shi X, Xu J, Yuan S, Zheng B, Zhang E, et al. Characterization of the genitourinary microbiome of 1,165 middle-aged and elderly healthy individuals. Front Microbiol. 2021;12:673969. Available from: https://doi.org/10.3389/fmicb.2021.673969
- Hrbacek J, Morais D, Cermak P, Hanacek V, Zachoval R. Alpha-diversity and microbial community structure of the male urinary microbiota depend on urine sampling method. Sci Rep. 2021;11(1):23758. Available from: https://doi.org/10.1038/s41598-021-03292-x
- Nickel JC, Stephens A, Landis JR, Chen J, Mullins C, van Bokhoven A, et al. Search for microorganisms in men with urologic chronic pelvic pain syndrome: a culture-independent analysis in the MAPP research network. J Urol. 2015;194(1):127-135. Available from: https://doi.org/10.1016/j.juro.2015.01.037
- Davasaz Tabrizi E, Sevil M, Arican E. Bioinformatic strategies in metagenomics of chronic prostatitis. World J Urol. 2025;43(1):188. Available from: https://doi.org/10.1007/s00345-025-05514-7
- Zheng Z, Hu J, Li W, Ma K, Zhang C, Li K, et al. Integrated microbiome and metabolome analysis reveals novel urinary microenvironmental signatures in interstitial cystitis/bladder pain syndrome patients. J Transl Med. 2023;21(1):266. Available from: https://doi.org/10.1186/s12967-023-04115-5
- Nickel JC, Stephens A, Landis JR, Mullins C, van Bokhoven A, Lucia MS, et al. Assessment of the lower urinary tract microbiota during symptom flare in women with urologic chronic pelvic pain syndrome: a MAPP network study. J Urol. 2016;195(2):356-362. Available from: https://doi.org/10.1016/j.juro.2015.09.075
Figures:
Similar Articles
-
The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain SyndromeMohammed Amine Elafari*,Mohammed Amine Bibat,Mamad Ayoub,Amine Slaoui,Tarik Karmouni,Abdelatif Koutani,Khalid Elkhader. The Urinary Microbiome: Shifting Paradigms from Sterile Urine to Microbial Dysbiosis in Chronic Pelvic Pain Syndrome. . 2026 doi: 10.29328/journal.ijcmbt.1001036; 9: 022-026
Recently Viewed
-
Myxedema Coma and Acute Respiratory Failure in a Young Child: A Case ReportRinah Elaisse R Dolores, Marion O Sanchez*. Myxedema Coma and Acute Respiratory Failure in a Young Child: A Case Report. Ann Clin Endocrinol Metabol. 2023: doi: 10.29328/journal.acem.1001027; 7: 008-013
-
Unveiling Disparities in WHO Grade II Glioma Care among Physicians in Middle East and North African (MENA) Countries: A Multidisciplinary SurveyFatimah M Kaabi,Layth Mula-Hussain*,Shakir Al-Shakir,Sultan Alsaiari,Leonidas Chelis,Renda AlHabib,Sara Owaidah,Renad Subaie,Marwah M Abdulkader,Ibrahim Alotain. Unveiling Disparities in WHO Grade II Glioma Care among Physicians in Middle East and North African (MENA) Countries: A Multidisciplinary Survey. Arch Cancer Sci Ther. 2026: doi: 10.29328/journal.acst.1001048; 10: 001-005
-
From Wallets to Waistlines: Exploring the Link between Family Income (Wage Distribution) and Obesity Indices in Pakistani PopulationsAtif Akbar,Waqas Ghulam Hussain*. From Wallets to Waistlines: Exploring the Link between Family Income (Wage Distribution) and Obesity Indices in Pakistani Populations. New Insights Obes Gene Beyond. 2026: doi: 10.29328/journal.niogb.1001024; 10: 001-014
-
Bacteriolysis Destruction for Cu- and Zn-Ions Induced Peptidoglycan Cell Wall Based on the Halo-test Results in Cu(NO3)2 and ZnSO4 Solutions against Staphylococcus epidermidisTsuneo Ishida*,Reiko Kobayashi. Bacteriolysis Destruction for Cu- and Zn-Ions Induced Peptidoglycan Cell Wall Based on the Halo-test Results in Cu(NO3)2 and ZnSO4 Solutions against Staphylococcus epidermidis. Int J Clin Microbiol Biochem Technol. 2026: doi: 10.29328/journal.ijcmbt.1001034; 9: 010-017
-
Germline BRCA1 Mutation inSquamous Cell Carcinoma of Oesophagus: Driver versus Passenger MutationAmrit Kaur Kaler*, Shraddha Manoj Upadhyay, Nandini Shyamali Bora, Ankita Nikam, Kavya P, Nivetha Athikeri, Dattatray B Solanki, Imran Shaikh, Rajesh Mistry. Germline BRCA1 Mutation inSquamous Cell Carcinoma of Oesophagus: Driver versus Passenger Mutation. J Genet Med Gene Ther. 2024: doi: 10.29328/journal.jgmgt.1001011; 7: 015-019
Most Viewed
-
Physical Performance in the Overweight/Obesity Children Evaluation and RehabilitationCristina Popescu, Mircea-Sebastian Șerbănescu, Gigi Calin*, Magdalena Rodica Trăistaru. Physical Performance in the Overweight/Obesity Children Evaluation and Rehabilitation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001030; 8: 004-012
-
Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging PresentationKarthik Baburaj*, Priya Thottiyil Nair, Abeed Hussain, Vimal MV. Hypercalcaemic Crisis Associated with Hyperthyroidism: A Rare and Challenging Presentation. Ann Clin Endocrinol Metabol. 2024 doi: 10.29328/journal.acem.1001029; 8: 001-003
-
Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trialSathit Niramitmahapanya*,Preeyapat Chattieng,Tiersidh Nasomphan,Korbtham Sathirakul. Effects of dietary supplementation on progression to type 2 diabetes in subjects with prediabetes: a single center randomized double-blind placebo-controlled trial. Ann Clin Endocrinol Metabol. 2023 doi: 10.29328/journal.acem.1001026; 7: 00-007
-
Exceptional cancer responders: A zone-to-goDaniel Gandia,Cecilia Suárez*. Exceptional cancer responders: A zone-to-go. Arch Cancer Sci Ther. 2023 doi: 10.29328/journal.acst.1001033; 7: 001-002
-
Ectopic adrenal tissue at the spermatic cordAbdallah Chaachou,Nizar Cherni,Wael Ferjaoui*,Mohamed Dridi,Samir Ghozzi. Ectopic adrenal tissue at the spermatic cord. J Clin Med Exp Images. 2022 doi: 10.29328/journal.jcmei.1001024; 6: 001-002

If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."